Search
- Page Path
- HOME > Search
Research Article
- [English]
- Association between nutrient intake and frailty status in Korean older adults: a cross-sectional study using the 9th (2022–2023) Korea National Health and Nutrition Examination Survey
- Hyejin Yu, Sang-Jin Chung
- Korean J Community Nutr 2026;31(2):153-164. Published online April 30, 2026
- DOI: https://doi.org/10.5720/kjcn.2026.00038
-
 Abstract
Abstract
 PDF
PDF - Objectives
This study evaluated the intake status of key macronutrients and micronutrients (calcium, magnesium, iron, and vitamin D) among Korean older adults and investigated their associations with frailty and its individual components.
Methods
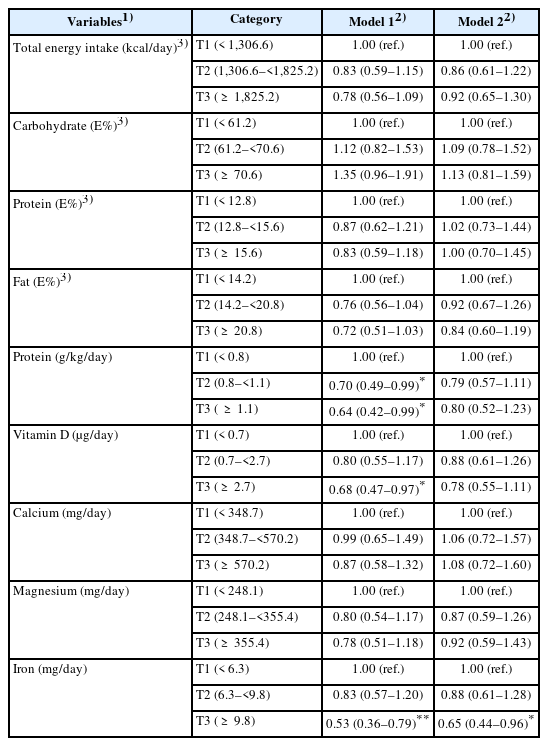
Data from 1,246 participants (aged ≥ 65 years) in the 9th Korea National Health and Nutrition Examination Survey (2022–2023) were analyzed. Participants were classified into Robust, Pre-frail, and Frail groups based on a modified version of the Fried frailty phenotype (unintentional weight loss, exhaustion/fatigue, muscle weakness, slow gait speed, and low physical activity). Nutrient intake levels were categorized into tertiles. Multivariable logistic regression was used to estimate odds ratios (ORs) for frailty. Model 1 was adjusted for age, sex, and total energy intake. Model 2 included additional adjustments for socioeconomic factors (household composition, household income) and function-related factors (aerobic physical activity, chewing difficulty, and disease status).
Results
Total energy intake differed significantly across frailty groups in both Model 1 (P = 0.011) and Model 2 (P = 0.043). In the fully adjusted model, participants in the highest tertile of iron intake (T3) had 35% lower odds of frailty compared to those in the lowest tertile (T1) (OR = 0.65; 95% confidence interval [CI], 0.44–0.96). Iron intake maintained the strongest independent association with reduced odds of muscle weakness (T3 vs. T1: OR = 0.45; 95% CI, 0.28–0.71). Furthermore, higher protein intake per kilogram of body weight (T3) was significantly associated with lower odds of slow gait speed (OR = 0.53; 95% CI, 0.33–0.87) in the minimally adjusted model. Vitamin D, calcium, and magnesium were not significantly associated with overall frailty after full adjustment.
Conclusion
Insufficient intake of protein and iron is associated with increased odds of frailty and its functional components in Korean older adults. These findings underscore the critical need for evidence-based nutritional interventions and policy development to prevent and manage frailty at the population level.
- 42 View
- 4 Download


 KSCN
KSCN
 First
First Prev
Prev